Por Diego Marcano
As the pandemic continues to evolve in cities and countries across the globe, queries about the novel coronavirus emerge every day. In Venezuela, questions of a deadlier coronavirus mutation arose after the government attributed the outbreak in the city of Maracaibo to a “much more aggressive virus.”
On May 29, 2020, the Sectoral Vice President of Communications, Culture and Tourism, Jorge Rodriguez, said the virus there had a “faster transmissibility with a high capacity of provoking symptoms in patients.” He did not provide specific information to back these claims.
Since the first case of COVID-19 was announced on March 13, Venezuelan authorities have reported 17.158 cases of COVID-19 and 156 deaths. The biggest outbreak has taken place in the state of Zulia, which borders neighboring Colombia.
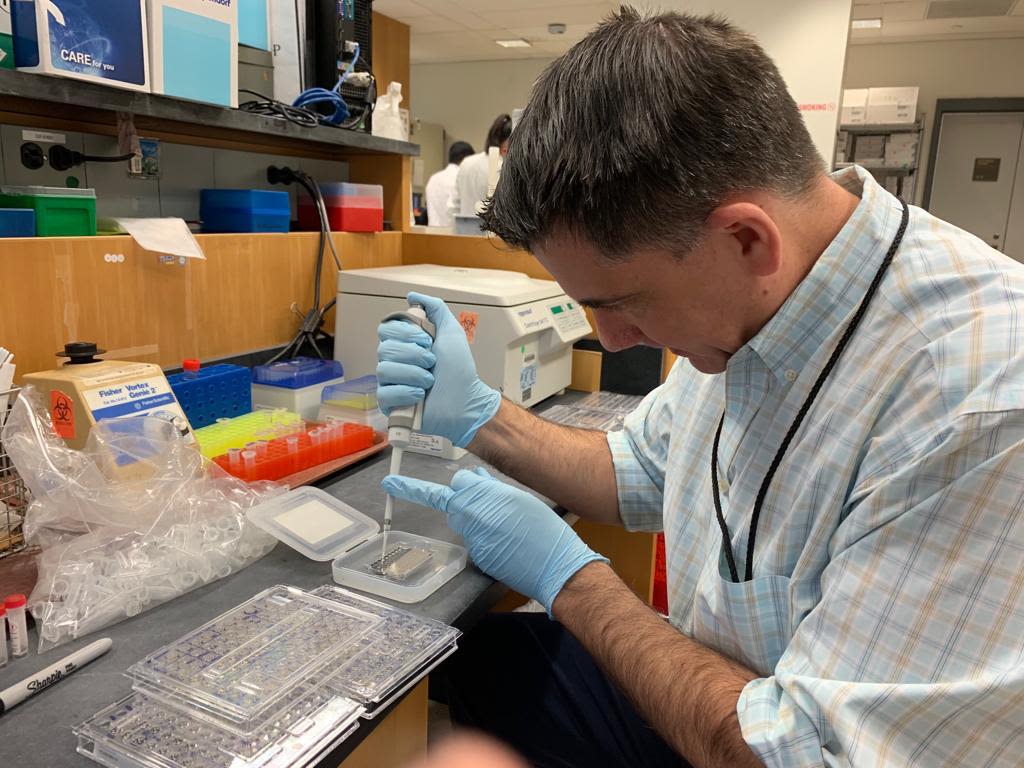
The first effort to find answers was carried out by a phylogenetic studies network, which includes Incubadora Venezolana, Universidad del Rosario and the University of Glasgow. In the study, scientists led by Dr. Paniz-Mondolfi from Mount Sinai Hospital in New York City, used nasopharyngeal clinical specimens from patients in bordering states to sequence the virus' genome.
The group sequenced three SARS-CoV-2 genomes from symptomatic Venezuelan patients and found “a point mutation in the Spike protein gene (D614G substitution), previously reported to be associated with increased infectivity, in all three Venezuelan genomes.”
“We managed to get three symptomatic patients, two in Cucuta who came from Tachira, and one in Cartagena coming from Zulia,” Dr. Paniz-Mondolfi said. “The mutational profile of the sequenced genomes from Venezuela revealed that three of the genomes were carriers of the substitution D614G, plus three additional mutations in one of the genomes.”
Dr. Paniz-Mondolfi from Mount Sinai Hospital in New York City. Photo courtesy of Alberto Paniz-Mondolfi.
Dr. Paniz-Mondolfi from Mount Sinai Hospital in New York City. Photo courtesy of Alberto Paniz-Mondolfi.
Paniz-Mondolfi said the Venezuelan Government has monopolized COVID-19 diagnosis and tightly controls access to samples. This prevents researchers from conducting the initial steps that would allow them to sequence the virus genome in the country.
“We can’t access that material in Venezuela,” Paniz-Mondolfi said. “Monopolizing epidemiologic information creates an obscurantism, sows doubt and distrust, which is not what the people need right now. This is the time for open science. Scientific collaboration efforts are what have stopped this pandemic from reaching the disproportionate levels of death that decimated the world’s population during the Spanish Flu.”
The new coronavirus is an RNA virus, which means that it’s a group of genetic material packed in a protein shell. And like most RNA viruses, it mutates rapidly.
After the virus comes into contact with a host, it starts making copies of itself to infect other cells in the body. When this happens, the virus makes mistakes in its genome. Those changes can pile up and then be placed in future copies of the virus, resulting in new mutations. This always occurs and mutations progressively accumulate as the virus continues to spread within the population.
Nonetheless, coronaviruses are an exception among RNA viruses. The coronavirus has a proofreading system that allows it to correct mistakes as it replicates. Thus regulating replication fidelity.
“That’s why it is said that the mutational activity of the coronavirus is rather moderate. However, it still has mutational activity,” Dr. Paniz-Mondolfi said. “Most mutations are neutral, meaning they won't fundamentally change the traits of the virus. But others might not only account for diversity and regional variation of the virus but could also affect its infectivity, pathogenicity and transmissibility.”
RNA viruses, such as measles and the flu, are more likely to produce changes and mutations in comparison with DNA viruses like smallpox, the human papillomavirus (HPV) and herpes, which often mutate at a slower rate.
“The mutation rate of this coronavirus ends up being about 30 mutations in the genome per year,” said Benjamin Neuman, head of the biology department at Texas A&M University-Texarkana. Neuman has studied coronavirus for over 20 years, he now has a youtube channel where he answers questions about COVID-19, and was part of the International Committee that named SARS-CoV-2.
“We're about six or seven months in, so we must have about 15 to 18 mutations now, compared to the virus you would get from the beginning of January or the end of December,” Neuman said.
Among the coronavirus mutations so far identified by scientists, the D614G mutation (the same that was found in the three genomes from Venezuelan patients) seems to be the one that has generated more concern. It was first documented on April 30, in a study by a group of scientists from Los Alamos National Laboratory, based in New Mexico, U.S.
Los Alamos National Laboratory in New Mexico. Photo from the official Facebook page.
Los Alamos National Laboratory in New Mexico. Photo from the official Facebook page.
In this study, the scientists, led by Dr. Bette Korber, looked at mutations affecting the virus’ protein spikes, which are used to recognize and invade the body’s cells. Using data from amino acid changes in the virus’ spike protein, the study shows how the D614G spike mutation quickly became dominant around the world, after being first detected in Italy, on February 20.
The authors proposed the hypothesis that the rapid spread of this new strain of the virus likely suggests that the D614G mutation is more infectious than its predecessor, the original D614 from Wuhan, China.
The study concluded that “the mutation Spike D614G is of urgent concern; it began spreading in Europe in early February, and when introduced to new regions, it rapidly becomes the dominant form.”
A later study published on June 12 by Scripps Research, that has not yet been peer reviewed, showed that the mutation D614G increased the likelihood of infection by stabilizing the virus’ spike proteins. According to the study, each viral particle of the newly discovered mutation had close to five times more functional protein spikes to bind and fuse with the host’s cells.
One of the main researchers, Hyeryun Choe, said that the spike mutation D614G made the virus “10 times more infectious in the cell culture system that we used.”
Geneticists and epidemiologists have questioned the hypothesis that the D614G mutation became dominant because it is more infectious, and point out that there is no evidence of a more severe disease linked to this mutation.
In a recent paper published in the scientific journal Cell, researchers Nathan Grubaugh from Yale University, William Hanage from Harvard University, and Angela Rasmussen from Columbia University, cited studies with data from hundreds of COVID-19 patients in London and Seattle, WA., and 88 patients from Chicago, IL.
Their analysis points out that patients infected with the strain of the virus containing the D614G mutation had higher viral loads. However, there was no significant difference in hospitalization outcomes, which would suggest that the mutation doesn’t necessarily lead to more severe disease.
“It’s impossible to conclude that a single mutation alone would have a major impact in a large, diverse human population based on in vitro infectivity and fitness data,” the paper reads. “Current evidence suggests that D614G is less important for COVID-19 than other risk factors, such as age or comorbidities.”
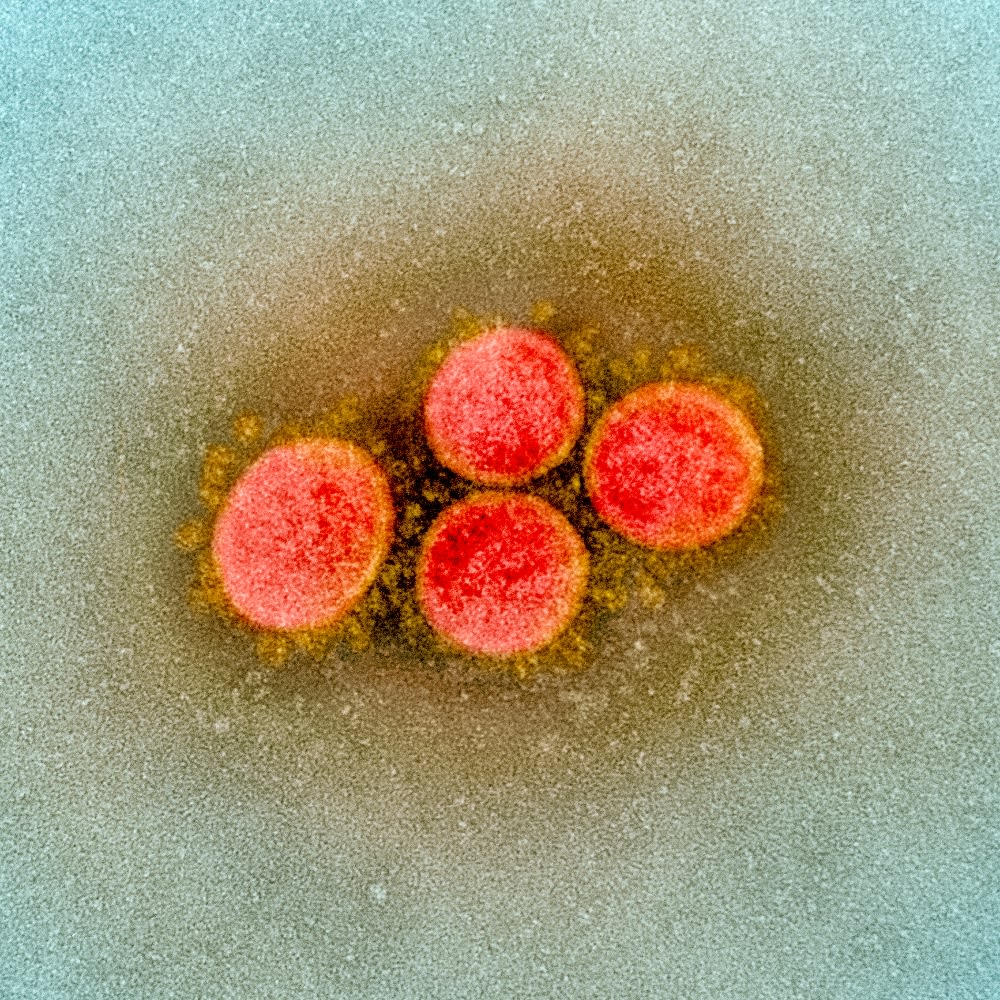
A transmission electron microscope shows SARS-CoV-2, taken from a patient. Photo: National Institute of Allergy and Infectious Diseases | AFP
A transmission electron microscope shows SARS-CoV-2, taken from a patient. Photo: National Institute of Allergy and Infectious Diseases | AFP
Vineet Menachery, of the University of Texas Medical Branch, is one of a few dozen virologists in the world who specialize in coronaviruses. He explained that the coronavirus overall doesn’t change much over time.
“It's not like a flu, where the antibodies that you generate won't actually protect you the next year,” Menachery said. “What's important is that whether you have the G or the D mutation, the disease outcome is not different. It's not a virus that's more deadly. It could be more transmissible but it doesn't appear to be that much more transmissible.”
Dr. Paniz-Mondolfi explained that tracking mutations is essential to guide the efforts to deal with the pandemic, as mutations may not only help assess the virus’ virulence or transmissibility, but it may also affect the accuracy of COVID-19’s diagnosis.
“We need to keep feeding our database with genomes and evaluate in real time how these mutational changes in the genetic makeup of the virus to monitor the performance of our diagnostic platforms,” Paniz-Mondolfi said.
The Venezuelan Institute for Scientific Research (IVIC) is currently sequencing SARS-CoV-2 genomes from different areas in Venezuela and is expected to report results soon.
Another concern is the impact mutations could have in the development of a vaccine against the novel coronavirus.
Mark Schleiss, a professor at the University of Minnesota Medical School and researcher with the Institute for Molecular Virology at the University of Minnesota, has spent 30 years studying vaccines and his lab has been working on coronavirus vaccines for the past months.
“It is important to determine the rate of the virus’ mutations, as well as keep track of the changes, as they can potentially affect the efficacy of vaccines and treatments.” Dr. Mark Schleiss said.
As with most things about the new coronavirus, mutations (and their potential effects) are being studied while the pandemic is still undergoing in many places around the world.
The best way scientists have to spot mutations or genetic changes in the virus is by comparing all the genes in different samples. Back in January, there was only one whole SARS-CoV-2 genome to study. Since then, researchers worldwide have built a collaborative database that compiles around 67,000 genomes of the novel coronavirus. In May, there were 50,000 genomes in the database and 70 percent of them had the D614G mutation.
New genomes are added every day from all over the world and each time a new one arrives they are thoroughly examined.
Over 90 vaccines and 50 antibody-therapeutics are being developed in different laboratories across the world in response to the pandemic. Most of these efforts target precisely the spike protein discovered in the original Wuhan reference of the virus, the one that in many places around the world now contains the D614G mutation.
As the virus propagates human-to-human and more mutations appear in its genome sequence, there is increased risk that these mutations could modify the virus in a way that might render a vaccine ineffective.
Bioinformatic tools such as Nextstrain and Pangolin are being used to track changes in the virus and enable the testing of mutations. The ultimate goal is to make sure that therapeutic treatments and vaccine development don’t suddenly stumble onto a mysterious mutation.
“I don't think that we need to let the idea of mutations change the way we deal with this virus,” Dr. Neuman said. “This virus is quite serious and we are finding new bad effects of the virus on children and on other healthy people almost every day. What I think we need to do is get together as a world and drive this particular virus to extinction.”
Credits
Graphic design: John Fuentes
Editors: Valentina Oropeza, Ángel Alayón y Oscar Marcano
Photography: National Institute of Allergy and Infectious Diseases, Luis Bravo | AFP
Translation: Diego Marcano
Caracas, 31 de julio de 2020